02 Apr Cephalometric Radiography: Essential Orthodontic Treatment Planning and Analysis
Cephalometric radiography stands as the cornerstone of orthodontic diagnosis and treatment planning, providing standardized lateral and posteroanterior views of craniofacial structures that enable precise analysis of skeletal relationships. This specialized imaging technique utilizes a cephalostat to ensure reproducible positioning and consistent magnification, making it indispensable for modern orthodontic practice.
Understanding Cephalometric Imaging Technology
Cephalometric radiographs are obtained using specialized equipment called a cephalostat, which maintains a fixed distance between the X-ray source and the patient’s head. This standardization ensures that measurements remain consistent across different time points, allowing orthodontists to track treatment progress and growth changes accurately. The transition to digital cephalometry has revolutionized this field, offering enhanced image quality, reduced radiation exposure, and streamlined workflow integration.
Lateral vs Posteroanterior Cephalometric Analysis
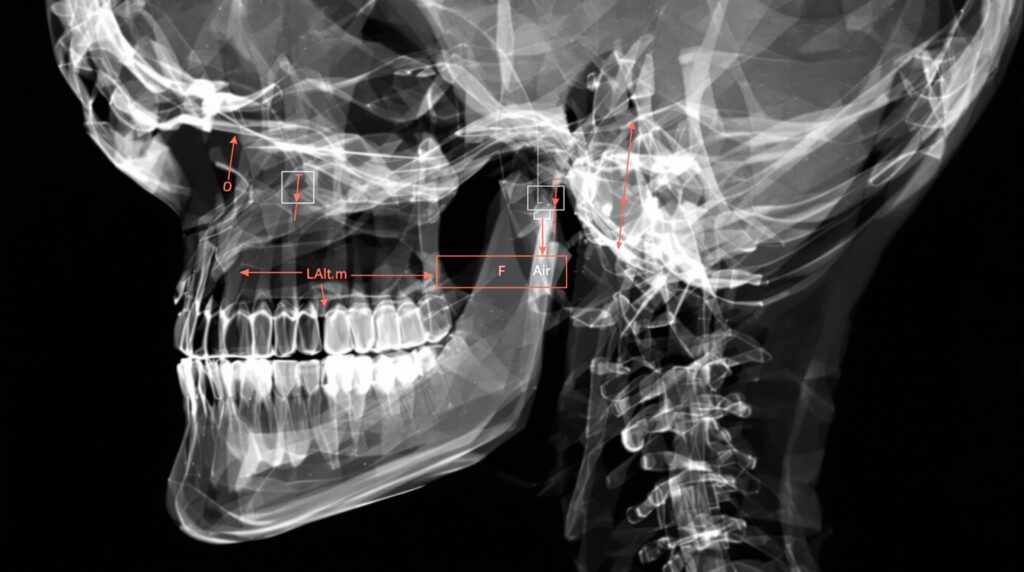
The lateral cephalometric radiograph serves as the primary tool for orthodontic analysis, providing detailed information about anteroposterior and vertical facial relationships. These images allow evaluation of maxillary and mandibular positioning, dental inclinations, and soft tissue profiles. Key anatomical landmarks such as sella, nasion, orbitale, and pogonion form the foundation for comprehensive cephalometric analysis.
Posteroanterior (PA) cephalograms, while less commonly used in routine practice, provide valuable insights into transverse facial dimensions and asymmetries. These frontal projections are particularly useful when evaluating patients with facial asymmetries, crossbites, or when planning surgical interventions that require assessment of facial width relationships.
Clinical Applications and Treatment Planning
Modern cephalometric analysis relies on established protocols such as the Steiner analysis and Downs analysis, which provide normative values for various angular and linear measurements. These standardized approaches help orthodontists determine skeletal classification, evaluate growth patterns, and develop appropriate treatment strategies for individual patients.
Digital Integration and Future Developments
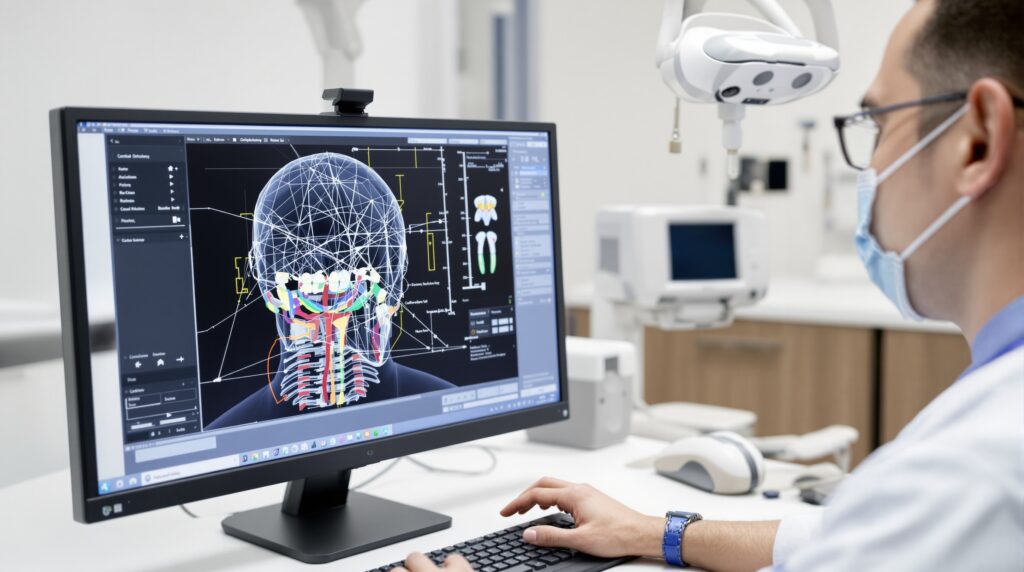
The integration of CBCT technology with traditional cephalometric imaging has opened new possibilities for three-dimensional analysis. CBCT-synthesized lateral cephalograms can successfully replace conventional 2D radiographs while providing additional volumetric information for complex cases. This advancement allows practitioners to maintain familiar analysis protocols while gaining enhanced diagnostic capabilities.
Artificial intelligence and automated landmark detection are transforming cephalometric analysis, reducing measurement errors and improving efficiency. These technological advances promise to make cephalometric evaluation more accessible and accurate, supporting better treatment outcomes for orthodontic patients.
Best Practices and Clinical Considerations
Proper patient positioning remains critical for accurate cephalometric imaging. The Frankfort horizontal plane should be parallel to the floor, with the patient’s head stabilized using ear rods and a nasion positioner. Consistent technique ensures reliable measurements and enables meaningful comparison between serial radiographs throughout treatment.
Radiation safety considerations mandate judicious use of cephalometric imaging, following ALARA (As Low As Reasonably Achievable) principles. Digital systems have significantly reduced radiation exposure compared to conventional film-based techniques, making routine monitoring more feasible while maintaining diagnostic quality.



Sorry, the comment form is closed at this time.