
11 Feb Understanding AI in Dental Imaging: How Artificial Intelligence Is Changing Radiograph Analysis
Artificial intelligence is rapidly transforming dental imaging. From detecting early-stage cavities that the human eye might miss to analyzing complex 3D CBCT scans, AI-powered tools are becoming a practical reality in dental practices around the world. But what exactly can AI do today, where are its limits, and what should dental professionals understand about this technology?
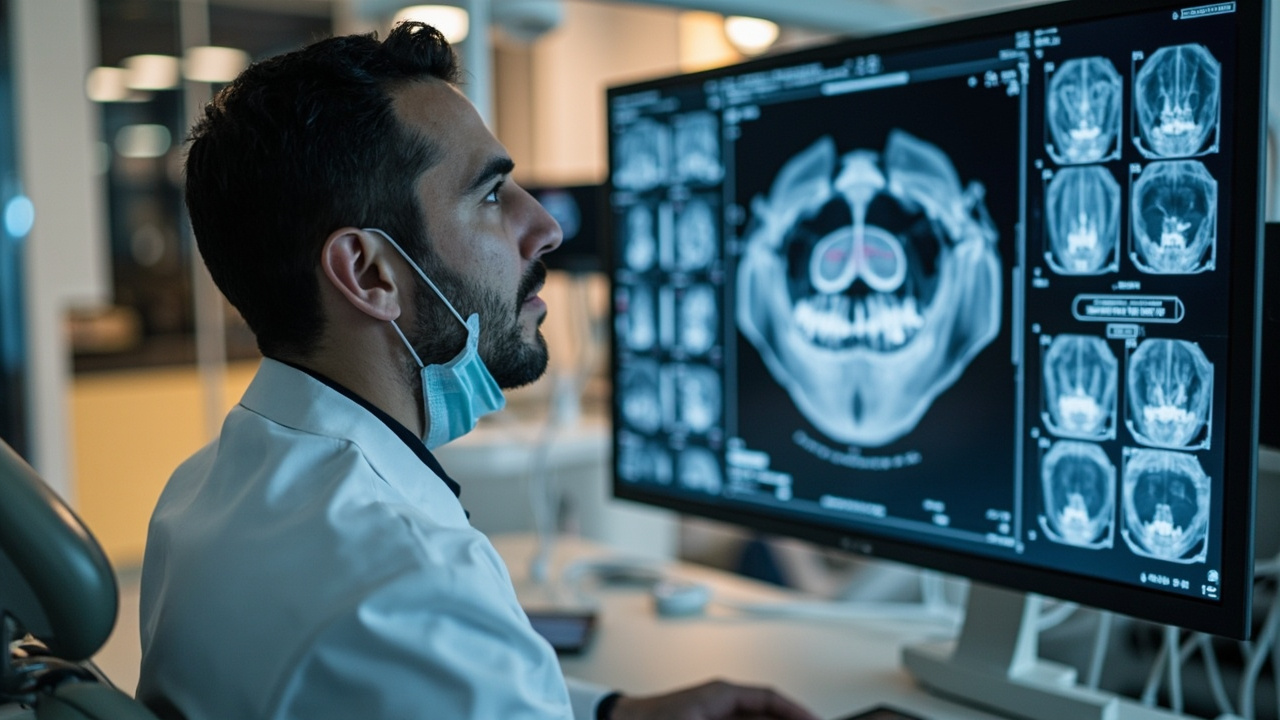
How AI Analyzes Dental Radiographs
AI systems designed for dental imaging use deep learning — a type of machine learning that trains neural networks on thousands or millions of labeled images. After seeing enough examples of healthy teeth, carious lesions, bone loss patterns, and periapical pathology, these systems learn to identify similar patterns in new images.
The process typically works like this:
- A digital radiograph (periapical, bitewing, or panoramic) is captured as usual
- The image is sent to the AI software — either integrated into your imaging software or as a cloud service
- The AI analyzes the image and highlights areas of concern, often with color overlays or annotations
- The dentist reviews the AI findings alongside the original image and makes clinical decisions
What AI Can Detect
Current AI dental imaging systems have demonstrated capability in detecting:
- Dental caries — AI excels at identifying interproximal caries, including early lesions that may be subtle on bitewing radiographs. Studies have shown AI can match or exceed average clinician detection rates for caries.
- Periodontal bone loss — AI can measure and map alveolar bone levels across the entire dentition, providing consistent quantitative assessments that support periodontal diagnosis and treatment planning.
- Periapical pathology — Periapical radiolucencies indicating infection, granulomas, or cysts can be flagged automatically, ensuring they’re not overlooked on busy days.
- Calculus detection — Some systems identify subgingival and supragingival calculus deposits on radiographs.
- Tooth numbering and anatomy — AI can automatically identify and number teeth, map restorations, and note missing teeth — saving time on charting.
- Endodontic assessments — Root canal quality, missed canals, and fractured instruments can be flagged for review.
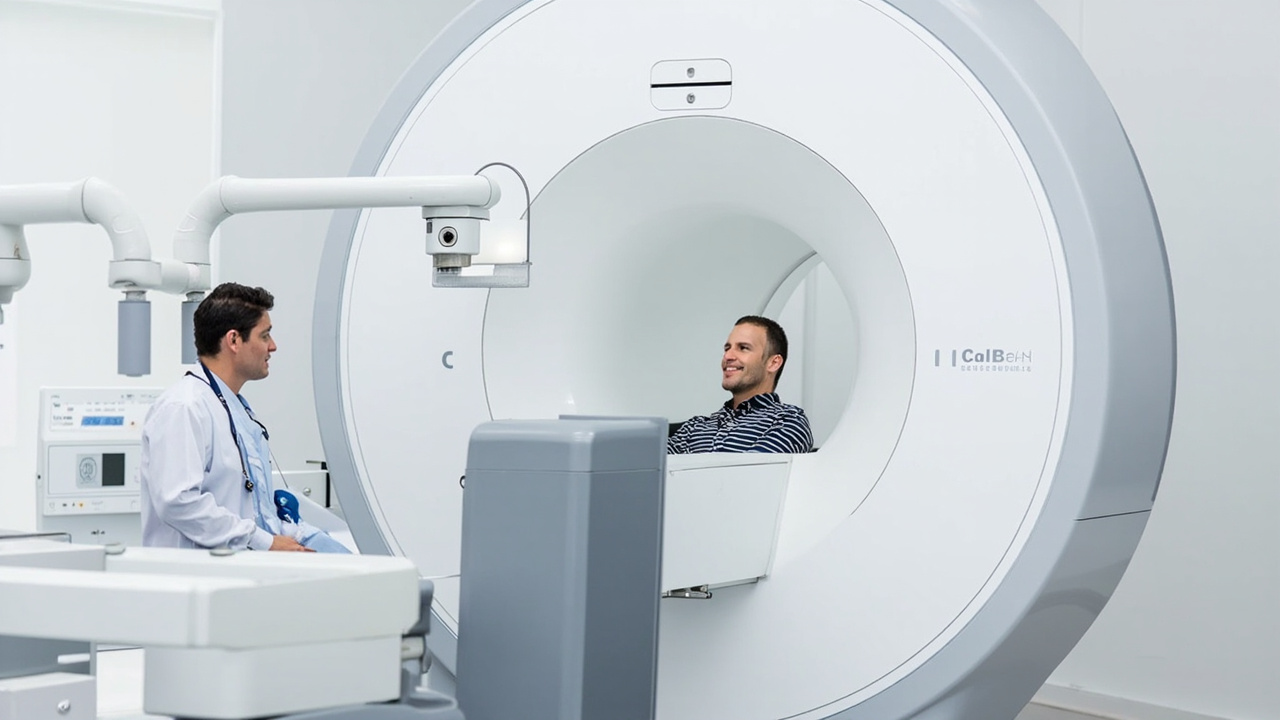
AI and CBCT: The Third Dimension
Cone beam computed tomography (CBCT) produces hundreds of cross-sectional slices that clinicians must scroll through manually. This is time-consuming, and subtle findings can be missed — especially outside the region of immediate clinical interest.
AI applications for CBCT are addressing this challenge:
- Airway analysis — AI can segment and measure the airway from CBCT volumes, supporting sleep apnea screening and orthodontic treatment planning.
- Implant planning — AI-assisted tools can identify available bone, map the inferior alveolar nerve, and suggest optimal implant positioning.
- Pathology detection in full volumes — AI can scan the entire CBCT volume and flag incidental findings in the sinuses, cervical spine, or areas outside the primary region of interest.
- Segmentation — Automated segmentation of individual teeth, nerves, and bone structures speeds up surgical planning and communication with patients.
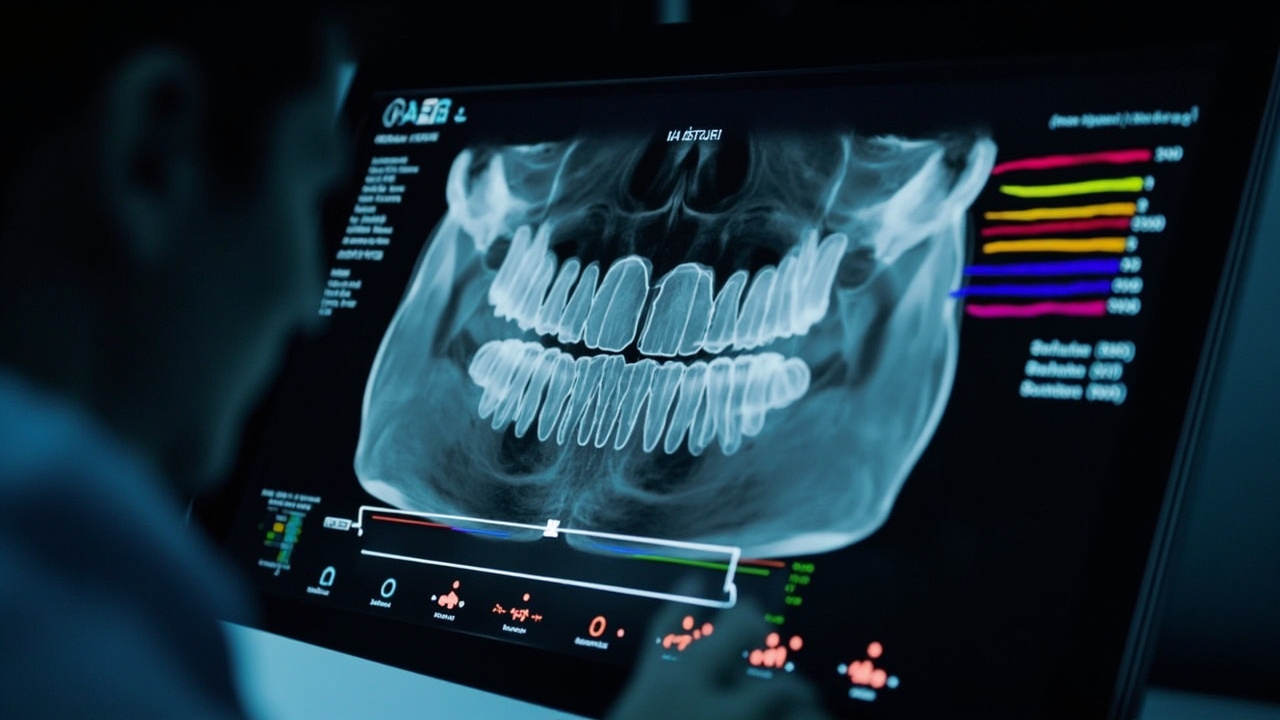
Benefits for Dental Practices
The practical advantages of AI-assisted imaging include:
- Consistency — AI doesn’t have bad days, fatigue, or distractions. It applies the same analytical rigor to the last patient of the day as to the first.
- A second set of eyes — AI serves as a diagnostic safety net, catching findings that might otherwise be missed.
- Patient communication — AI-generated visual overlays make it easier to show patients exactly what’s happening in their mouth, improving case acceptance.
- Efficiency — Automated charting and detection can reduce the time spent on image analysis, particularly for panoramic and CBCT studies.
- Documentation — AI annotations create a detailed record of findings at the time of image capture.
Limitations and Important Considerations
AI is a powerful tool, but it has real limitations that every dental professional should understand:
- AI assists — it doesn’t replace clinical judgment. AI systems are designed as decision-support tools. The final diagnosis always rests with the clinician, who has access to clinical examination findings, patient history, and context that AI cannot see.
- False positives and false negatives occur. No AI system is 100% accurate. Over-reliance on AI without clinical correlation can lead to overtreatment (false positives) or missed pathology (false negatives).
- Image quality matters. AI performance depends on image quality. Poorly exposed, poorly positioned, or artifact-laden images will produce unreliable AI results — garbage in, garbage out.
- Training data bias. AI systems are only as good as the data they were trained on. If training datasets underrepresent certain populations, tooth morphologies, or pathology types, the AI may perform less reliably in those cases.
- Regulatory landscape is evolving. AI dental imaging products must be cleared by regulatory bodies (FDA in the US, Health Canada). The regulatory framework for AI in healthcare is still maturing.
- Cost considerations. Most AI imaging services require monthly or per-image fees. Practices need to evaluate whether the clinical and efficiency gains justify the ongoing cost.
The Road Ahead
AI in dental imaging is not a future concept — it’s here today, with products from companies like Overjet, Pearl, Dentistry.AI, and others already in clinical use. As the technology matures, we can expect improved accuracy, broader integration with existing imaging and practice management software, and new applications we haven’t yet imagined.
For dental professionals, the key is to approach AI as what it is: a sophisticated tool that enhances your clinical capabilities without replacing them. The best outcomes will come from clinicians who understand both what AI can do and where its limitations lie — and who use it as one more instrument in their diagnostic toolkit.



Sorry, the comment form is closed at this time.